When MCAS-Like Symptoms Aren’t MCAS: Hidden Dental Infection and Other Upstream Drivers
For clinicians and deeply curious readers who want a systems-based breakdown of secondary mast cell activation, differential diagnosis, and the history clues that change the case.
When MCAS-Like Symptoms Aren’t MCAS: Hidden Dental Infection and Other Upstream Drivers
For clinicians and deeply curious readers who want a systems-based breakdown of secondary mast cell activation, differential diagnosis, and the history clues that change the case.
What MCAS actually means
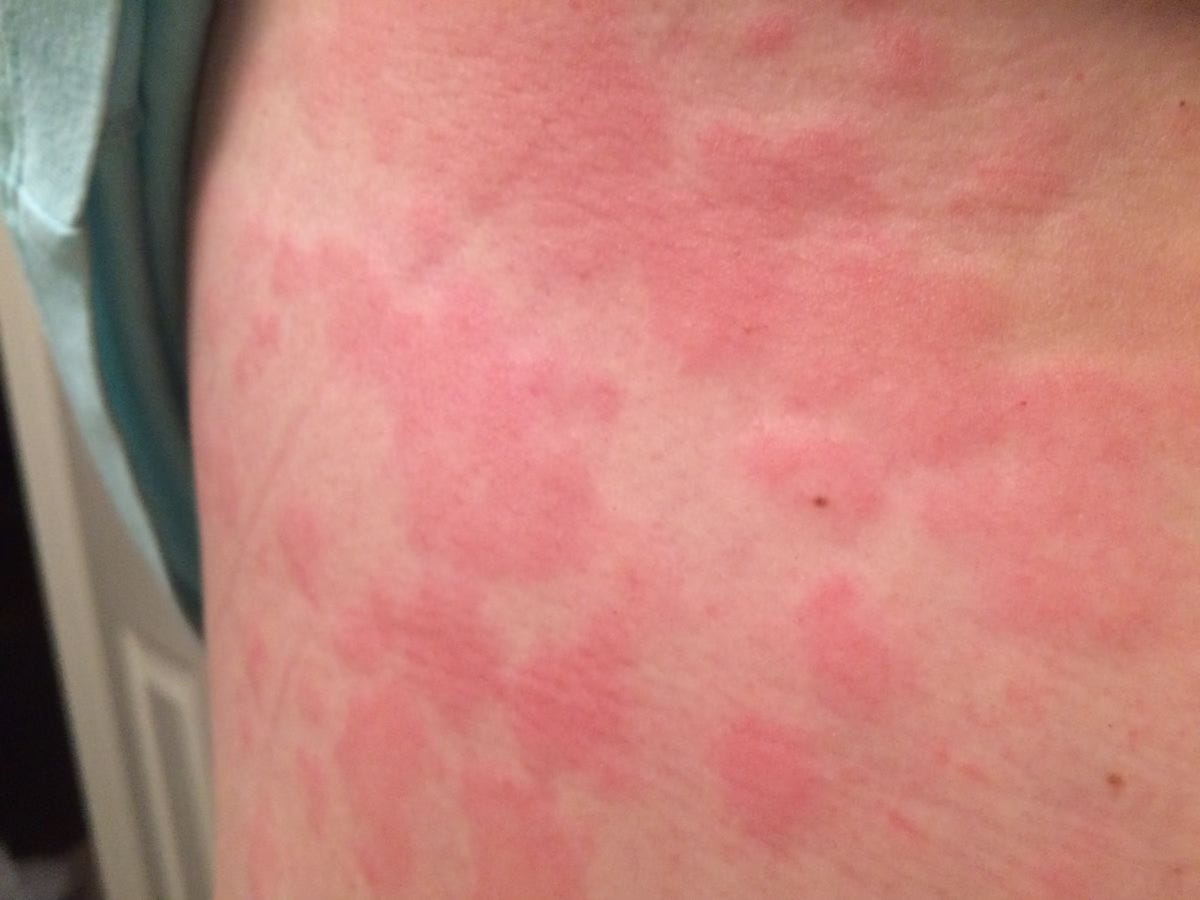
Mast cells are immune cells best known for their role in allergic reactions. When they release too many chemical mediators, people can develop symptoms like flushing, hives, swelling, rapid heart rate, wheezing, dizziness, nausea, vomiting, diarrhea, or crampy abdominal pain.
True MCAS is not just “I react to everything.” It is a specific diagnosis built on recurrent severe episodes, usually affecting at least two organ systems, with objective evidence of mast cell mediator release during an event and improvement with treatments that block those mediators.
When I say “MCAS-like symptoms,” I mean the patient looks mast-cell-driven on the surface, but the deeper question is still open. Is this true MCAS? Secondary mast cell activation from an upstream trigger like infection, allergy, or a medication reaction? Or another mimic altogether? That distinction is the entire point of this article.
The mistake that keeps complex cases stuck
Not every histamine-heavy, multisystem flare is true MCAS. And not every hidden inflammatory problem announces itself where the symptoms are loudest. Current guidance treats MCAS as a specific syndrome, with a prototypical presentation of severe, episodic symptoms typical of mast cell activation affecting at least two organ systems, plus objective evidence of mediator release and response to mast-cell-directed treatment. Infections, meanwhile, are recognized causes of secondary mast cell activation.
That distinction matters because many patients arrive already organized around the wrong frame. They have real symptoms, often severe. They have already tried the usual route for a mast-cell-heavy presentation: trigger avoidance, diet changes, gut protocols, hormone work, nervous system work, symptom management, maybe a growing list of supplements and restrictions. Relief is partial, inconsistent, or absent. The label gets stronger while the case gets murkier.
This article is not arguing that MCAS is not real. It is arguing for a cleaner differential. Some patients have true consensus MCAS. Some have secondary mast cell activation. Others have an MCAS-like presentation driven by an upstream problem that never should have been left off the map in the first place. Recent practical guidance specifically recommends excluding secondary causes before landing on MCAS, and it warns against broad symptom-based overcalling.
The case behind this piece is a good example of why that matters. By the time she got to me, she had already done the obvious symptom-centered work. Nothing meaningful was changing the case. That matters, because nonresponse is data. If the basic framework is not moving the patient, the answer is often not a more intense version of the same framework. Sometimes the job is not to suppress the flare better. Sometimes the job is to ask what is recruiting the flare in the first place.
Why this pattern is easy to miss
One reason cases like this get missed is that people expect dental pathology to be obvious. They picture severe tooth pain, facial swelling, or a clean dental complaint. But apical periodontitis is an inflammatory disorder of the tissues around the root tip caused by persistent microbial infection in the root canal system, and it can be symptomatic or asymptomatic. Chronic or asymptomatic lesions can still contribute to systemic inflammatory burden.
Then add bruxism. Cracked teeth can cause erratic pain with chewing, sensitivity to hot or cold, and symptoms that come and go, enough that even the treating dentist may have difficulty localizing the tooth. An abscessed or infected tooth may also be painful, but it may not be.
That is exactly why history-taking matters. As I took her history, one detail stood out: she clenched and ground her teeth. There was no big dental complaint. No obvious signpost. No classic presentation that would make everyone immediately say, “look in the mouth.” But the detail was enough to move oral pathology higher on my map.
So I suggested something simple and appropriately conservative: if she had not had routine dental X-rays recently, ask her hygienist whether she was due. That is not a recommendation for random imaging. FDA guidance is clear that radiographs should be individualized and used when the expected diagnostic yield will affect care. But once the history makes oral pathology plausible, the mouth belongs in the workup.
The pivot
Then the case turned.
Her tooth cracked. Imaging was done. It revealed a large hidden infection.
Once the infected tooth was removed, the entire MCAS-like picture resolved, which completely changed the differential. The symptoms were real. The suffering was real. But the label was incomplete.
That does not mean mast cells were irrelevant. It means the cleaner interpretation was secondary mast cell activation, or an MCAS-like inflammatory presentation driven by an occult dental source. AAAAI specifically notes that infections can activate otherwise normal mast cells through “secondary activation,” and current guidance emphasizes ruling out secondary causes before concluding MCAS.
This is not a tooth story, it is a systems story
The lesson here is not that teeth are the hidden answer to every complex patient. The lesson is that mast-cell-looking symptoms are often downstream, and multiple systems can create a very similar clinical picture. Practical MCAS guidance explicitly recommends considering other diagnoses, such as chronic spontaneous urticaria or carcinoid syndrome in the right context, and then exploring secondary causes of mast cell activation such as food allergy or NSAID hypersensitivity before assigning the label.
So the principle is bigger than the mouth. Oral health is one example. Another patient’s upstream driver might live in allergy, medication reactions, airway and sleep load, gastrointestinal disease, autonomic strain, infection, or another inflamed system entirely. The point of systems medicine is not to guess a favorite root cause. It is to widen the lens until the pattern makes sense.
Why this matters
This matters because labels control attention. Once a patient is framed as “MCAS,” “histamine,” “gut,” or “hormones,” every new symptom gets interpreted through the same lens. The risk is not only missing the diagnosis. The risk is missing the chance for source control. And in dentistry, an untreated abscess or root infection is not a philosophical issue. It needs treatment, and untreated infection can spread.
A respectful root-cause approach still has to know when to escalate. Facial swelling, fever, rapidly worsening pain, foul drainage, trouble swallowing, or trouble breathing require urgent dental or emergency evaluation.
If this reframes a case you keep seeing, send it to the clinician who still assumes the loudest symptom points to the primary problem.
In the members-only section, I map the full systems picture behind this pattern, show how I separate true MCAS from secondary mast cell activation and MCAS-like mimics, walk through the anatomy and physiology of bruxism, tooth cracking, apical infection, mast-cell activity, sleep, autonomic load, and inflammatory burden, break down the symptom clusters and exam findings that matter most, and finish with a short case vignette that shows the exact pivot point where the plan changed.
Paid members get every weekly Root Cause Breakdown, the full archive, and a voice in what we cover next.